Are you a Nurse preparing for your licensing exams? This article is all about Primary Hyperaldosteronism, also known as Conn’s syndrome. The content is for general information but mainly focused on nurses preparing for their licensing exams including NCLEX-RN, DHA, MOH, HAAD, and Prometric.
The content is for general information but mainly focused on nurses preparing for their licensing exams including NCLEX-RN, DHA, MOH, HAAD and Prometric. The nursing management revolves around monitoring the blood pressure and complications related to hypokalemia and providing interventions to manage blood pressure and potassium levels as well as preparing the client for adrenalectomy if indicated.
Primary Hyperaldosteronism (Conn’s Syndrome)
Today we are talking about primary hyperaldosteronism which is also known as Conn’s syndrome. Even before we go to the topic and we start talking about what is hyperaldosteronism you need to understand that we have got two adrenal glands situated on top of each kidney.
Hyperaldosteronism is characterised by excessive secretion of aldosterone, which causes an increase in sodium reabsorption and loss of potassium and hydrogen ions. Primary hyperaldosteronism is caused by a problem with one or both adrenal glands which is characterised by hypernatremia, hypokalemia and alkalosis.
What does the adrenal gland do?
Before when we try to understand what the adrenal gland does, we need to understand that the adrenal gland has two parts to it. One is the adrenal medulla which is the inner portion and another part is the outer portion which is known as the adrenal cortex.
Today we will be talking about primary hyperaldosteronism we are going to be more focused on the adrenal cortex because the adrenal cortex is the area from where aldosterone gets released. There are many other hormones that get released from the adrenal cortex such as you have cortisol and many other hormones. But in today’s session, we would be talking about aldosterone and will be focusing on aldosterone which is basically Mineralocorticoids. And the other kind of corticoid is a glucocorticoid that is again secreted by the adrenal cortex.

What does aldosterone do?
Well, in short, aldosterone is responsible for balancing the Sodium and potassium levels of the blood. So this is the primary function of aldosterone. Still, also aldosterone plays an indirect role in maintaining the pH of the blood. A direct role in maintaining the Sodium and Potassium balance and an indirect role in maintaining the pH of the blood.
What are the triggers for aldosterone release?
When does aldosterone get released? Well, basically there are two triggers. One is Angiotensin II. Now if you can recollect about angiotensin II, I am not going to detail this because we can do the details in another section. But in short, we are talking about angiotensin II, we need to remember that this is part of the renin-angiotensin mechanism. So if the pressure of the blood goes low, so rated as low BP, then the renal blood flow also falls, the renal blood flow also decreases. Now as the renal blood flow decreases the juxtaglomerular cells of the kidney detect this and secrete renin.

Well, now when it’s secrets renin what happens is renin is responsible for converting Angiotensinogen to Angiotensin I. Angiotensin I is then converted to Angiotensinogen II under the influence of the angiotensin-converting enzyme.
What is angiotensin II?
Now what is angiotensin II? Angiotensin II does two things.
One is it causes vasoconstriction. So since it causes vasoconstriction, is going to increase the blood pressure or in other words normalise the blood pressure. So our problem was that the blood pressure was low. So here we have increased or brought back the blood pressure to normal with the help of angiotensin II.
Another function of angiotensin II is to stimulate the release of aldosterone a star hormone for the day. So this is why I mentioned that one of the triggers for aldosterone release is angiotensin II. So what is the second trigger? The second trigger is increased potassium in the blood. So whenever there is an increase in potassium levels in the blood you can expect the release of aldosterone. Specifically, because aldosterone is responsible for maintaining the Sodium and Potassium balance.
What does aldosterone do and how does it work?
So now we come to the next question: what does aldosterone do and how does it work? So before we even begin to understand the condition we need to understand where aldosterone work and how it works. Well, aldosterone works on the late distal convoluted tubule. So this particular area is the late distal convoluted tubule also known as a DCT and this is specifically known as the late distal convoluted tubule. So late distal convoluted tubule is one area where aldosterone works.
Now the second area where aldosterone works is the common collecting tubule. So these are the two areas where aldosterone primarily works. Now let’s take a closer look at the cells of these two areas. We have got the special cells known as principal cells. These principal cells are basically lining the late distal tubule and the common collecting ducts. So that are the principal cells. This is the blood vessel that runs parallel to the principal cell and more specifically we will call this peritubular capillary. So peritubular capillaries if you can recollect in the diagram of nephron the blood vessels which are going around these collecting tubules. So these are peritubular capillaries.
What do peritubular capillaries do?
Peritubular capillaries are responsible for the reabsorption and secretion of substances into the nephron and out of the nephron. So that’s what this blood vessel represents.
We know from previous knowledge that blood is abundant in sodium whereas cells are abundant in potassium. This does not mean the only ions inside the arm cells there is Sodium also but in comparison to Sodium Potassium ions are more in cells and in comparison to potassium sodium ions are more in the blood. Now the cell has to maintain this balance of sodium and potassium.
So how does it do it? It does it through something known as a Sodium Potassium pump. So you got this pump on this principal cell. What does this pump do? It takes in 2 potassium ions and gives 3 sodium ions. So this is how this pump works. Take 2 potassium ions inside and give 3 sodium ions into the arm blood. This is how the sodium-potassium levels in the blood and the cells are maintained.
What happens if there is an increased amount of potassium in the blood?
Well, if there is an increasing amount of potassium in the blood from the previous slide we know that aldosterone release takes place. Now, what does aldosterone do? So that is the aldosterone star of the day and that aldosterone acts on this Sodium Potassium pump. And what does it do? It stimulates the Sodium Potassium pump to work harder. Now the Sodium Potassium pump is going to work harder under the influence of aldosterone. This means that it’s going to take more potassium inside and throw out more sodium outside. But you need to remember that we are talking that there is increased potassium in the blood. For potassium to come inside sodium has to go into the blood. From somewhere inside the cell you need to get sodium. Now we know that this is the area where urine is passing.
Now urine is abundant in sodium. This means that if this sodium can come into the cell, the intracellular sodium levels can increase. This means that this pump can effectively full potassium. So aldosterone creates a channel. What channel? A sodium channel. Now, what does the channel do? It does the obvious. It pulls in the sodium from the urine into the cell. Also, we know that this pump is going to pull in a lot of potassium into the cell and as time passes by what can happen is the amount of potassium in the cell can increase. So somebody has to remove it.
Aldosterone does another thing. It creates another channel which is known as the potassium channel. And again it does the obvious, is going to remove excess potassium into the urine. So all in all aldosterone is helping the Sodium Potassium pump to work harder. How it helps it to work harder is by creating two channels so that sodium can be pulled inside the cell and can go to the blood and potassium can be pulled from the blood taken into the cell and then thrown out into the urine. Now you can appreciate the fact that aldosterone is important for maintaining the Sodium and potassium balance. And this is how it does it under normal circumstances.
What happens if the aldosterone levels are very high?
Unnecessarily aldosterone is released by the adrenal gland. This process of potassium removal and gain of sodium is going to be exaggerated. That’s going to increase. something is going to happen. Now you can see that all of that sodium that was in the urine is absorbed and sent to the blood and all of the potassium that was there has been thrown out into the urine. This can happen when the levels of aldosterone are too high even if there are unwanted amounts of aldosterone. And hence we come to the conclusion that if there are high levels of aldosterone then the blood is going to lose potassium and gain Sodium and water. Now, this is obvious because more amount of sodium in the blood is going to lead to more amount of water getting pulled into the blood.

In short, if there is increased aldosterone, abnormally high levels of aldosterone that going to lead to reduced potassium levels in the blood and increased sodium levels in the blood, increased blood volume. These are the three important things or three main problems that can happen if there is an abnormal increase of aldosterone. All the other things that you would see as technical manifestations would be related to these three cardinal incidents that are happening.
Aldosterone indirect function – Primary Hyperaldosteronism
Let’s move to the next where we are also going to discuss in short an indirect function of aldosterone. The previous function was the direct function and here we have an indirect function. Alpha intercalated cells are present in the Kidney and the main function of an Alpha intercalated cell is to get rid of acid from the blood. So again the blood vessel or specifically the peritubular capillaries and we know that there are hydrogen ions. So we know that there are protons in the blood and we need to get rid of these. We need to get rid of these hydrogen ions to maintain the acid-base balance. So this is also an Alpha intercalated cell and this space between the cell where urine is flowing.
So now we know that normally all cells make carbon dioxide and water. Now, why do they make carbon dioxide and water for their metabolic purposes they are going to break down the carbohydrates and then the end product is going to be carbon dioxide and water. Now, this carbon dioxide and water are going to react with carbonic anhydrase which is basically an enzyme and that’s going to get converted to one hydrogen ion and one bicarbonate. So here you see that one Proton is there and here also you have one hydrogen. you need to get rid of these from the cells because they are acidic.
How do we get rid of that? Well, we get rid of that through a Transporter. This is the Transporter. What the Transporter does is it takes out the bicarbonate and in exchange, it takes in a chloride ion from the blood. Now in the blood what happens? You got rid of one Proton, remember that’s gone. Now you just have one remaining. Here you had these protons. This is going to undergo a reverse reaction. So bicarbonate is going to react with the hydrogen ion there and will form carbon dioxide and water. Well, water is in the blood, it is going to be thrown out after some time when it reaches the Kidneys to urine. Carbon dioxide will be thrown out through your lungs when this blood is going to reaches the lungs. So what have you done? You got rid of water and carbon dioxide.
Another transporter takes back chloride into the blood vessel. So here you can see from the blood also we got rid of hydrogen ion, from the cell also we got rid of one proton. But still, you need to remember that there is another proton that is remaining inside. And as time passes by, the number of protons is going to keep on rising. Now what’s going to happen is there is another channel or in other words a transporter that’s going to be acted upon by aldosterone. So aldosterone is going to help this transporter to remove the excess protons from the cell. So here you see that now our cell is free of protons or excess hydrogen ions and this excess hydrogen ion is thrown out into the urine.
It’s done by this channel but indirectly aldosterone is helping this transporter to work better. That is why I mentioned it indirectly plays a role in maintaining the acid and base balance or to speak specifically it indirectly helps in removing the excess hydrogen ions that keep piling up inside the cells.
What may happen if there are extremely high levels of aldosterone?
Simple, if there are excessively high levels of aldosterone, there is a higher chance that more amount of hydrogen ions are going to be thrown out into the urine. This means that you are going to go into a state where there is alkalosis because there is a loss of hydrogen and the loss of protons. So this is how hyperaldosteronism or expressively high aldosterone can also lead to alkalosis. Now I hope that this concept of what aldosterone does and what can happen if there is excess aldosterone is very clear. Because once you get these concepts right rest of it is going to be a piece of Casey.

What is primary hyperaldosteronism?
Now we come to the topic of primary hyperaldosteronism also known as Conn’s syndrome. Basically, this is hyposecretion of aldosterone.

What causes hypersecretion of aldosterone?
Why and what causes hypersecretion of aldosterone? It’s usually an adenoma. So usually what happens is if there is a tumour on the adrenal gland that will lead to excess secretion of aldosterone leading to primary hyperaldosteronism.
What can happen if there is excess secretion of aldosterone?
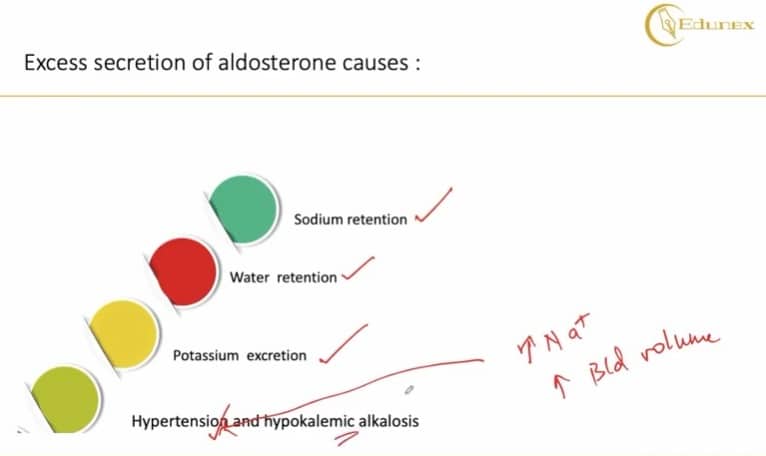
It can lead to sodium retention, we saw that it can lead to water retention, it will lead to potassium excretion, it will lead to hypertension because of the increased sodium levels, increased blood volume all this is going to lead to hypertension and it can lead to hypokalemic alkalosis.
What are the assessment findings?
The assessment findings are all the symptoms will be related to hypokalemia, hypertension and hypernatremia. So your clients can have a headache, fatigue, muscle weakness, cardiac dysrhythmias, paraesthesia, tetany, visual changes, glucose intolerance and elevated serum aldosterone levels. All of these symptoms that you have seen are directly related to hypokalemia because you know that Potassium is very important for Muscular contraction and relaxation. It has an effect on the cardiac muscles as well as you could see all of these symptoms. Of course, you will be able to see a lot of hypertension and increase BP in these patients and also glucose intolerance.
We do not know the exact reason why glucose intolerance can occur but it is believed that when there are high levels of aldosterone it affects the insulin level. The insulin levels are affected and that is why the client gets glucose intolerance, that is what is believed to be happening.

Primary Hyperaldosteronism – Nursing interventions
Let’s look at the nursing interventions. so I think by now you got a hang of what is hyperaldosteronism and its symptoms. So, of course, the main and the most important thing is to monitor the vital signs, especially the blood pressure, you will have to monitor the potassium and sodium levels, and you will have to monitor for hyperkalemia. We were talking all through this session about hypokalemia.
You will have to monitor for hyperkalemia if your patient has impaired renal function. So you know if there is impaired renal function then that potassium which is being thrown out into the urine is still inside the body, it’s technically not going out. So your patience is not going to show hypokalemia. So there can be a very high chance of hyperkalemia. So if there is impaired renal function do check for hyperkalemia. If there is excess potassium intake check for hyperkalemia.
So if you find your patient is hypokalemic and you are giving him potassium supplements, you need to monitor if he is developing hyperkalemia. If he is on potassium diuretics, then direct at all its potassium retaining it is not allowing the potassium to exit from the body. So there can be increased amounts of potassium. You need to look out for hyperkalemia.
If the patient is on an aldosterone antagonist, it’s an antagonist, it is acting against aldosterone. So when it is acting against aldosterone it is not allowing potassium to be thrown out into the urine. It is causing potassium to build up in the blood. So that’s what an antagonist does. It works against aldosterone. If your patient is on an aldosterone antagonist, also you need to monitor or check if the patient is developing hyperkalemia. Administer potassium supplements as prescribed and depending upon the blood levels of potassium.
Prepare the client for adrenalectomy
And finally, prepare the client for adrenalectomy because most of the time the cause of primary hyperaldosteronism is a tumour on the adrenal gland and it’s important that you either remove the tumour as fast as possible or you have to remove that entire adrenal gland. I am not going into details of adrenalectomy. Let’s keep that for another session.
So that is pretty much about what is primary hyperaldosteronism. Just to check whether you have understood these, I have put a question in front of you. You can read the question, understand the question and in your mind think about what could be the answer.
Infographic Primary Hyperaldosteronism

- The Key Foods For Mental Health | Harvard Nutritional Psychiatrist
- Anti Aging Foods That Will Keep You Young And Healthy
- What Are The Best Foods For Sound Sleep Through The Night
Question – Primary hyperaldosteronism
A nurse taught a client about the dietary changes required to manage Hyperaldosteronism. The nurse determines that the client understands the information presented if the client states a need to decrease which type of food?
- Oranges
- Red meats
- Salty snacks
- Whole-grain breads
Did you get the answer? The answer is Salty snacks because salty snacks are high in sodium. And a problem with hyperaldosteronism is that you already have hypernatremia. You don’t want to give a lot of salty snacks and not the patient again. So you would understand that the client has understood what is hyperaldosteronism if the client states that I am not going to take any salty snacks.
Final Thoughts
Hope that I could cover everything you need to learn about Primary Hyperaldosteronism. As a nurse, you must have thorough knowledge about what, causes, treatment, and nursing management of each and every disease. Your proper care is very important for the patient. Treat all patients as your family member and give proper care. Your consoling and encouraging words and proper care will help to ease the pain and speedy recovery.
Thank you for the visit. Hope you enjoyed your reading.
Kindly share this article on your network and help others to read it.
Please leave your views about this article in the comments box and don’t forget to subscribe to this site.
Reference for additional reading: https://www.emedicine.medscape.com/article/127080-overview
References: YouTube Rinta Rajan

Mathukutty P. V. is the founder of Simply Life Tips. He is a Blogger, Content Writer, Influencer, and YouTuber. He is passionate about learning new skills. He is the Director of PokketCFO.
He lives with the notion of “SIMPLE LIVING, CREATIVE THINKING”. He Believes – “Sharing is caring.” and “Learning never ends.”



